Platelet-Rich Plasma (PRP) Injection Therapy
Your own blood can help heal your body.
What is PRP Therapy?
This advanced biocellular injection therapy regulates inflammation, stimulates repair, and promotes remodeling of damaged tissues.
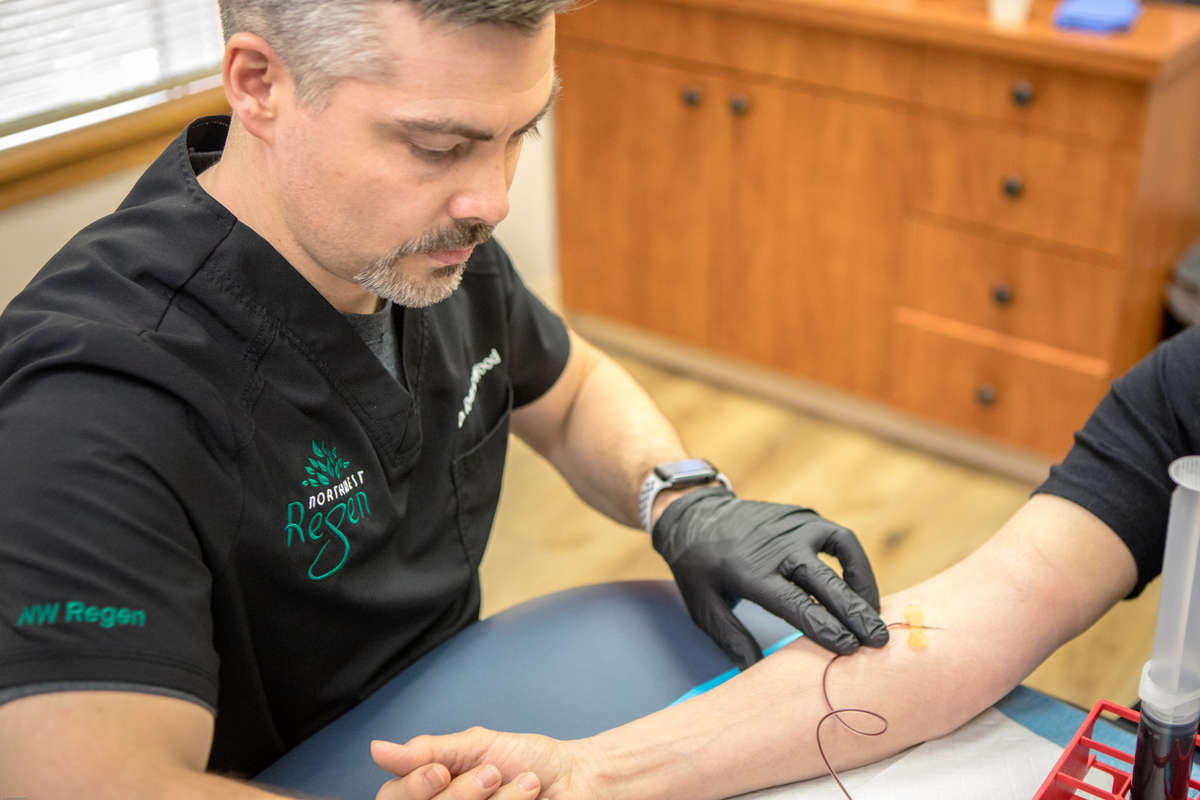
We begin with a simple blood draw processed in our in-office lab under highly specialized protocols to produce platelet-rich plasma (PRP) tailored to you. Then administer a PRP injection directly to the painful area to promote repair and healing, using precise ultrasound to visually guide the injection.
How do PRP injections work?
Injecting a platelet-rich solution directly to the injured tissue promotes the healing process. Platelets form the first line of defense in response to tissue damage. They contain α-granules rich in growth factors and cytokines that promote tissue regeneration, healing and repair.
What conditions do PRP injections treat?
- Chronic joint pain and instability
- Degenerative osteoarthritis in joints
- Sprains, strains, and other sports injuries
- Meniscal Tears
- Rotator Cuff Tears
- Calcific Tendinosis
- Frozen Shoulder
- Chronic Tendinitis
- Plantar Fasciitis
- Dry-Eye Syndrome
- Men and women’s sexual health
- Hair loss in both men and women
Platelet-Rich Plasma (PRP) Injection Therapy FAQs
What is Platelet-Rich Plasma (PRP)?
Once red and white blood cells are removed from blood using a centrifuge, the yellowish liquid left behind is called plasma. When properly processed in our lab, this plasma contains proteins, fibrinogen, glucose, clotting factors, and concentrated platelets.
How do you make PRP?
Why do we use Platelets for healing?
Does PRP vary?
What is the proper dosage of Platelets?
Does the baseline vary from person to person?
How do I know if I’m getting the baseline?
Why should I choose NW Regen for my PRP treatment?
We use an in-house lab to customize our PRP process, so we know exactly the number of platelets you have and can determine exactly the volume of whole blood needed to tailor any of the desired levels of platelets to achieve optimal healing. Not every condition requires the same procedure, and what works for you may not work for someone else.
Does PRP have any adverse reactions?
The only adverse reaction reported is transient pain and localized swelling after injections, with overall adverse reactions being very low. The other risk factor with any interventional procedure is infection, which we minimize by using sterile aseptic techniques.
Nguyen, C., & Rannou, F. (2017). The safety of intra-articular injections for the treatment of knee osteoarthritis: a critical narrative review. Expert Opinion on Drug Safety, 16(8), 897–902.doi:10.1080/14740338.2017.1344211
Articles about Platelet Rich Plasma
Role of Regenerative Medicine in Chronic Pain Relief ~ Surgery Isn’t the Only Option
For many patients struggling with chronic pain, surgery is often seen as the only way out. ...
The Hidden Connection Between Stress and Strength
Explore the Link Between Men's Mental Health and Physical Health You pride yourself on being...
Need to Prep for Ski Season But Too Sore From Summer? Learn How Regenerative Injections Can Help
September can sometimes still feel like summer in Portland—but fall is around the corner! If...